Within minutes of its appointment, a shot was fired across the bow of the new Health Care Delivery Review Committee reminding us, lest we had forgotten, of the trials of bringing change to the public health sector.

(Courtesy nwrha.co.tt)
In condemning Committee chairman Dr Winston Welch, former Health Minister Dr Fuad Khan cast his objection in the political terms of a PNM campaign against “UNC doctors.” But Dr Welch and his team should have enough experience to know that even the noisiest politics is no match for the far more serious money interests which are strangling the public health system.
It is not that we don’t know the problems or are unfamiliar with their causes and symptoms.
Starting with the Moyne Report of 1946, every review of the public health sector has described a comprehensively inadequate state of affairs in recommending more resources, better management and greater accountability for delivering anything approximating quality health care.
Since the last report submitted in 2009 by the Gafoor Commission of Enquiry, the only things likely to have changed might be the names and faces of betrayed patients and the bank accounts of those with a major investment in keeping the public health system dysfunctional.
Today, we are long past the old problem of individual fortunes being built on the backs of a broken public health system.

(Copyright Trinidad Guardian)
Thanks to a combination of ineffective policy and emboldened political investors, the roles are now fully reversed. The public health system now exists at the mercy of private suppliers of goods and services while the private health sector has grown into a full-fledged, highly integrated industry whose survival no longer depends on an ailing public health system even if its enrichment always will.
Six years ago, the Gafoor report had turned up enough information about phantom companies operating in the health sector along with accounting discrepancies to prompt then Prime Minister Patrick Manning to send the findings to the Director of Public Prosecutions.
If anything ever came out of that, it must’ve occurred outside of the public eye.
Since then, the problem has spiralled with taxpayers now paying twice for the same health service.
At least, this is the impact of the previous government’s policy of paying private hospitals to fill gaps in the public health system even as it finances the free public health system through taxes.

(Courtesy PAHO.org)
The Welch Committee can be in no doubt about the deep structural nature of the health sector’s problems which go well beyond the problem of personal culpabilities, as widespread as these might be. Interfere with one part of the problem and the whole thing could come crashing down.
Former Health Minister Hamza Rafeeq learnt this the hard way during the first Panday administration when his attempt triggered rebellion in the medical ranks that extended to a lengthy strike by nurses.
Right from the beginning, the best option for improving health care delivery has been the one least favoured by both government and medical professionals.
A public health system that rests on a decentralised base of well-resourced community hospitals linked to a modern local government system would be more manageable while spreading quality health care more evenly across the country.
Decentralised governance structures, however, are not features of the post-colonial world where the centralisation of power, and therefore of resources, has remained the dominant theme.
(Copyright BET)
Combine this with the insecurities that make us easy prey to global hawkers of dazzling mega projects and you begin to understand the crazy logic behind the decisions, particularly in health and education, that have both sectors in the mess they are today.
If the past 53 years have taught us anything it is the urgent need to complete the independence process by redistributing power into the hands of the people so that each one of us can share the responsibility for governing our communities and, by extension, our country.
In this, local government reform is a key strategy but its success will be determined by the extent to which the centre is prepared to devolve power and to which people are drawn into the process of government.
This is no overnight affair. It requires the budding of a new culture steeped in rational thought and which rejects the mindlessness of ethnic solidarity. The more we build our power systems around communities, the greater the chance that the national power system will reflect the reality of our lives on the ground.
Hopefully, in reviewing the national health care delivery service, the Welch Committee will focus on the underlying conditions that have allowed its problems to mushroom to today’s unmanageable proportions.

(Copyright fdslaw.com)
Hopefully, too, the committee will avoid the political pitfalls that could snuff it out even before it gets going. Having requested the review, it will be up to the Prime Minister to manage the political process once he gets the committee’s report.
Given the substantial health industry interests with no stake in change, the government’s greatest ally will have to be the public.
Without public support, Dr Keith Rowley might discover that winning an election is a cake walk compared to transforming the health sector.
Sunity Maharaj is a journalist with 38 years of experience and the managing director of the Lloyd Best Institute of the West Indies.
She is a former Trinidad Express editor in chief and TV6 head of news.
 Wired868 Wired868 for smart sport news and opinion
Wired868 Wired868 for smart sport news and opinion
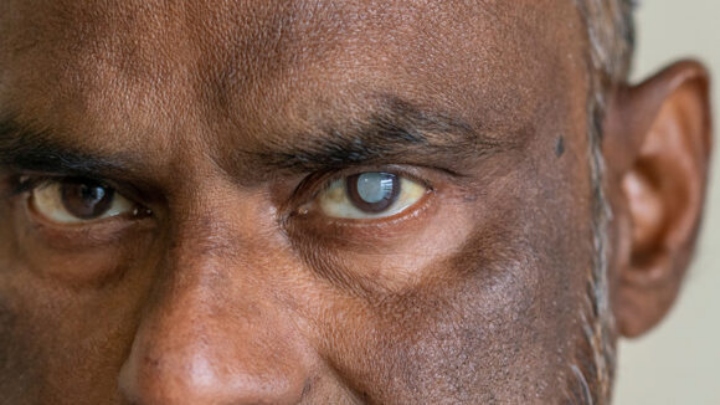





If you visit the WHO and CIA fact book sites and run a comparison among TnT, Estonia, Mauritius Swaziland the info is quite interesting. The 4 countries have similar populations. Mauritius and Singapore (5M population) became independent around our time and Estonia from the USSR in the 90s. Singapore is ranked near the top in the world for health care and other development indicators without having oil and minerals. We can’t blame our size nor that we are a young nation for our woes.
The PM should be praised for this bold step, but like Sunity says, we’ve been here before, lots of reports etc, and when it comes to implementation, few governments have been able to challenge the power that is the medical profession. Not all of them, but the ones who benefit from the public system being underdeveloped. Its sickening that we are in the top 10 globally for lifestyle diseases and still our healthy care ‘system’ remains curative at heart: so yes, nuff amputations, dialyssis, hypertension etc, but whosmanging these folks at a community level? Not community nurses in health centres helping and supporting patients to make better health choices, while managing a patient workload, but the same old general practitioners making tons of doling out very expensive pharmaceuticals. It is shameful that the politicians and the doctors between them have let the public down this way. But who’s making a fuss about public health care and decentralisation? Not many.
I don’t think the average layman understands the issues very well. And that doesn’t bode well for the “public support” that Sunity Maharaj feels the Prime Minister will need soon.
For most, the issues are just long lines and poor customer service. And possibly distance to travel too.
But then I suspect many lower middle class people and up have been forced to abandon public health care long ago.
Not to mention totally beholden to a the curative approach that only sees them when they develop somne chronic illness, with little management, little by way of follow up, tracking progress, interacting with professionals and paramedical health personnel at the community level, which is what we should have had ages ago, not the travesty that currently exists that stresses out people, doesn’t really help them, even, has them waiting long hrs to see a doctor who may not even turn up, because they might be running late working in their private practice etc.
It’s a very complicated situation – power struggles; incompetence; patronage; the omertà attitude of senior medical practitioners; the attraction of private sector pay checks for doctors who have made accountants their new best friends, etc. etc…..
I think the clannish behaviour of doctors would put even mob bosses to shame actually! I am not sure where to even start with this one.
Big issues!
It is a shame that we seem to be spinning top in mud. I submitted a complaint in the last commission of inquiry. I wrote to the then president GMR who never responded, then minister if health John Raphael who personally phone to apologize for the terrible treatment my pregnant wife and I received at the POSGH. I wrote to Families in Action they never responded. Anyway info is there for us to fix the system. But just like the judicial/crime/ justice system it is benefitting a few at the cost of the rest of the populace. Most people are getting their palms greased so nobody wants to call names or solve it because they will also be found wanting.